Beacon of the Cancer Care – From adressing cancer injustice to new patient centered, personalized, AI & data-driven horizons of oncology
he latest research from the World Health Organization’s (WHO) cancer agency, the International Agency for Research on Cancer (IARC) finds the global cancer burden is rising. The study, based on a survey of 115 countries, also finds a majority are failing to fully finance cancer treatment and palliative care for those with terminal cancers. And people in developing countries have worse outcomes after being diagnosed with cancer, it says. With millions of people losing their lives to cancer, the IARC survey finds a concerning lack of funding to care for those with cancer.
The report says; “only 39% of participating countries covered the basics of cancer management as part of their financed core health services for all citizens, ‘health benefit packages (HBP). Only 28% of participating countries additionally covered care for people who require palliative care, including pain relief”.
The burden of this shortfall in funding for adequate cancer care is not carried equally. The IARC survey finds what it calls “striking cancer inequity” across the developed world and emerging economies.

Europe’s Beating Cancer Plan is a political commitment to turn the tide against cancer and another stepping stone towards a strong European Health Union and a more secure, better-prepared and more resilient EU.
Following the publication of the new European Cancer Manifesto, EU lawmakers and stakeholders have driven home the importance of improving prevention and screening policies across Europe. As EU Beating Cancer Plan highlights, number of indicators show major differences in cancer prevention and care between and within Member States. These inequalities can be seen in access to prevention programmes, in rates of early cancer detection, diagnosis, access to treatment, survival and measures to improve quality of life of cancer patients and survivors. These inequalities are unacceptable in a European Health Union that seeks to protect everyone.

Addressing cancer has been one of the top political priorities during the past years, with initiatives like the BECA report from the European Parliament and the European Commission’s EU’s Beating Cancer Plan putting it high on the agenda.
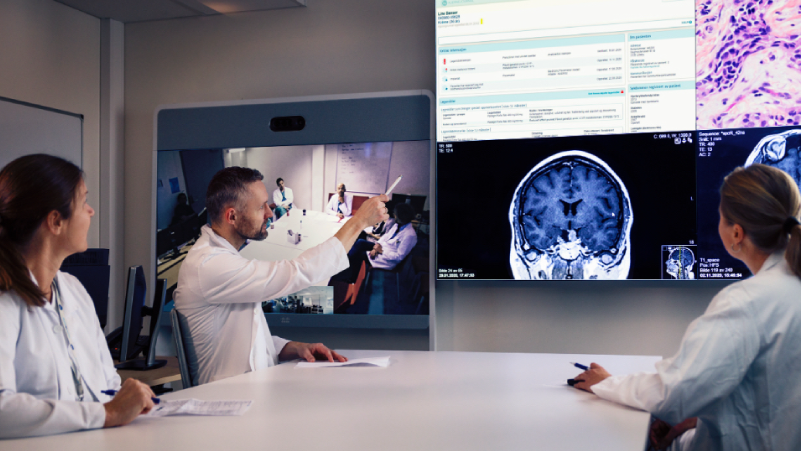
Also, the rapid rise of digital and data-driven technology in healthcare — such as artificial intelligence (AI), the Internet of things (IoT) and robotics — could offer unprecedented potential in the fight against cancer. The rise of computational tools has unlocked new approaches to treatments. In particular, AI and machine learning hold the potential to revolutionise how drugs are matched to patients, taking personalised cancer care to the next level. Such technologies could also drastically transform the timeline for developing new drugs, making it a matter of months rather than years. New digital technologies may transform health outcomes and support a better patient experience. A wide variety of established digital tools, often including mobile applications and telehealth, have been employed to help patients and families manage some aspects of cancer care from the relative comfort of their homes.
Emerging evidence even suggests that virtual reality could become a potential tool for cancer care across a variety of use cases, including patient education and anxiety management.
![]()
Personalized healthcare thrives on a comprehensive understanding of the patient, which is often compromised by the fragmentation of health data. Data silos in healthcare create a fragmented landscape of vital health information, hindering a comprehensive understanding of patient health and journeys. The journey to personalized healthcare is built on the interconnectivity of health-related data, requiring not only technological innovation but also a shift in data governance and culture. This transformation requires strict privacy standards, interdisciplinary and cross-industry collaboration, and a steadfast commitment to patient-centric values. The positive response to transparent data sharing in patient companion apps indicates a growing patient readiness for this evolving healthcare model, highlighting the importance of integrity and transparency in data use.
Following this, Health Hub would like to address those important issues with series of articles “Beacon of the Cancer Care” on the margins of HOK24 Oncology Congress. We kindly invite you to follow our series of articles in upcoming days.
REFERENCES //
https://www.who.int/news/item/01-02-2024-global-cancer-burden-growing–amidst-mounting-need-for-services
https://commission.europa.eu/strategy-and-policy/priorities-2019-2024/promoting-our-european-way-life/european-health-union/cancer-plan-europe_en
https://www.euractiv.com/section/health-consumers/news/prevention-and-screening-key-to-addressing-cancer-in-the-eu/
https://www.weforum.org/agenda/2023/06/digital-health-the-next-frontier-in-the-global-fight-against-cancer/
https://www.weforum.org/agenda/2024/02/personalized-healthcare-data/
Partners of “Beacon of the Cancer Care”