AmCham EU & Economist Impact Study: “At a turning point Healthcare systems in Central and Eastern Europe”
tudy „At a turning point: Health care systems in Central and Eastern Europe“ is conducted by Economist Impact and supported by AmCham EU. The study highlights key differences and commonalities in healthcare financing and policy approaches as governments rise to the challenge of managing the interlinked dynamics of population health, constrained resources and uncertainty following the COVID-19 pandemic and current economic slowdown.
As governments rise to the challenge of managing the interlinked dynamics of population health and economic uncertainty, At a turning point: Healthcare systems in Central and Eastern Europe highlights the key differences and commonalities in healthcare financing and policy approaches across 13 European countries. The report, written by the Economist Impact, identifies major trends and aims to benchmark access and provision of healthcare services, medicines, healthcare outcomes as well as quality of care. It also puts forward a number of recommendations for action, in areas such as financing models, delivery of care, access to innovative treatments, diagnostics and digital infrastructure.
Key objectives of the report was to raise awareness on health system dynamics in CEE , to generate the latest data and insights on health system financing, available resources, provision of care and health system efficiency and resilience and to identify priorities and a call to action for the selected CEE countries to support future direction and health system reform .
Key data sources: OECD, Eurostat, EFPIA, WHO, European Commission, Medicines for Europe, local statistical institutions and health authorities and interviews with local and regional experts ranging from policymakers, healthcare practitioners, health economists, and academics
A series of country profiles complement the study, featuring detailed data and additional analysis on the national dynamics. Country profiles are available for seven of the CEE countries: Bulgaria, Croatia, Czech Republic, Hungary, Poland, Slovakia and Slovenia. Romania has been included in this study as a comparator country.

Photo by Freepik
At a turning point: Healthcare systems in CEE
- Lower spending on healthcare in CEE countries has led to weak financial protection and high levels of unmet need – covid-19 has further exposed these weaknesses
- Current public financing models in CEE countries are no longer sustainable in the face of changing population demographics and rising economic uncertainty
- Hospital-centric care still dominates with less resources allocated to preventative and long-term care. Workforce shortages and migration also put current systems under pressure
- The promising pipeline of new innovative medicines provides an opportunity to transform how care is delivered – however in CEE fewer innovative medicines are available with longer wait times
- CEE countries falling behind other EU members in terms of readiness for digital adoption, the pandemic showed the need for rapid digitisation across the healthcare sectors.
Photo by Freepik
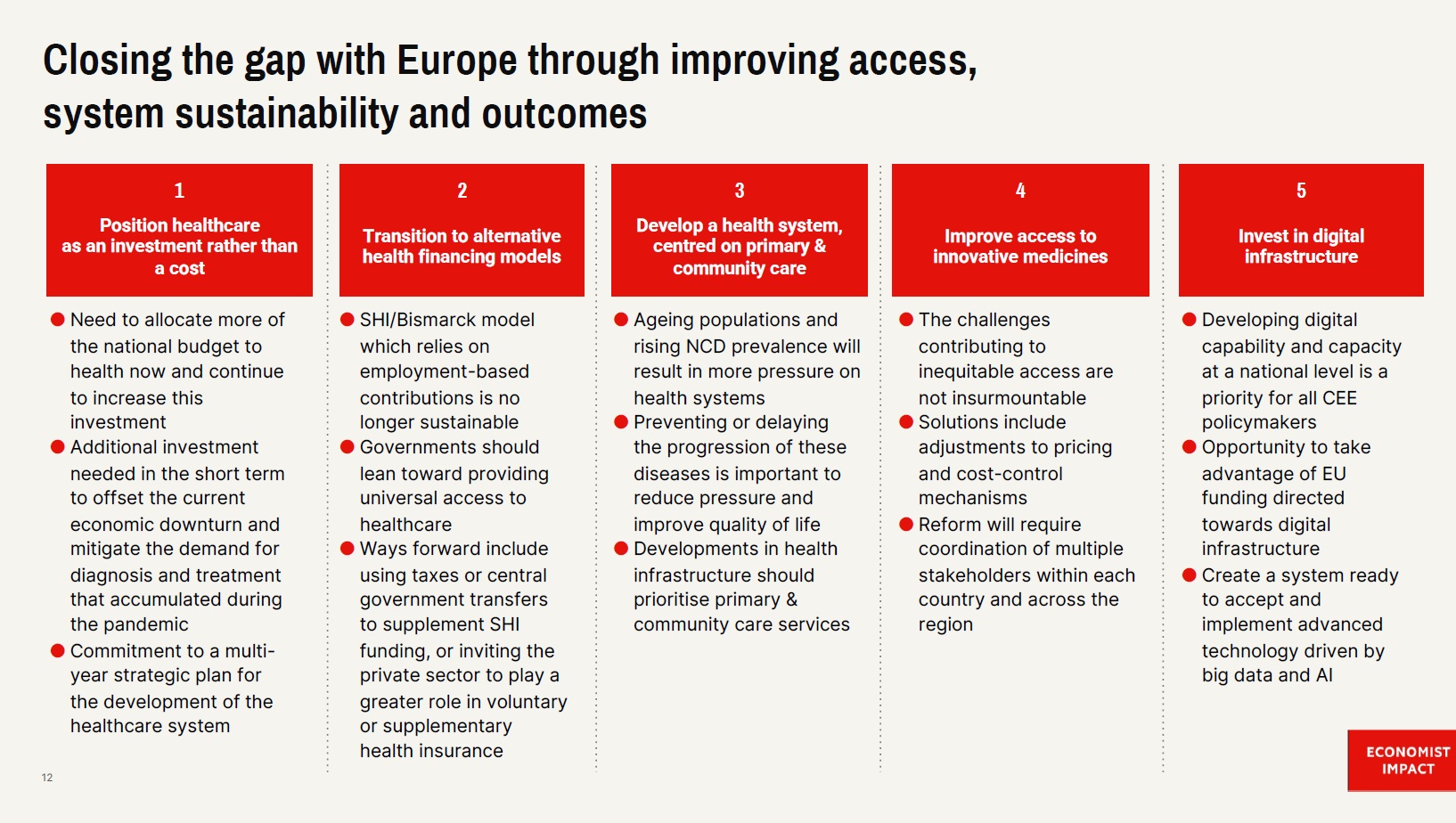
Call to action: Closing the gap through improving access, system sustainability and outcomes
1 / Position healthcare as a necessary investment that will support economic growth and lead to a more cost-effective health system in the future
2 / Transition from SHI to alternative health financing models that support universal access to healthcare
3 / Develop a health system, centred on primary & community care that meet the needs of future population and epidemiological demographics
4 / Improve access to innovative medicines through adjustments to pricing and cost-control mechanisms and coordination and transparency among stakeholders
5 / Invest in digital infrastructure through developing digital capability and capacity at a national level and take advantage of EU funding

Photo by Freepik
CEE countries lag behind the rest of the EU in terms of accessibility and availability of innovative medicines
The impact of new innovative treatments not reaching patients in CEE countries is likely to lead to higher mortality and avoidable deaths, lost quality of life and an increase in preventable healthcare costs
CEE countries allocate a higher proportion of their healthcare budget to medical goods
- However net spending per capita in euro terms is 2-3 times lower than the EU5 (1). Pricing and reimbursement policies in CEE have traditionally prioritised cost-containment
- Heavy focus on cost-containment measures regardless of the long-term benefit of new health technologies on healthcare costs and outcomes
- Pressure is growing on all governments to improve access to clinically effective innovative medicines for all prevalent diseases The EFPIA Patients W.A.I.T Indicator 2021 shows inequalities in patient access and disparities between east and west
- CEE countries have 23-55% of innovative medicines available while comparative EU countries have access to 51-91% of medicines (2)
- The average delay between market authorisation and patient access can vary by a factor greater than x7 across Europe – from as little as 4 months in Denmark to over 2.5 years in Romania2
- Root causes of access inequalities are multifactorial ranging from regulatory process delays, late initiation of reimbursement assessment, duplicative evidence requirements, reimbursement decisions delays, local formulary decisions and limited budget (3)
- EU policy reforms that aim to address patient access inequalities include the Pharmaceutical Strategy for Europe, EU HTA Regulation, Orphan Medicinal Products & Paediatrics legislation revision and the AMR Council Recommendations
Sources: 1. Eurostat. 2019, 2. IQVIA. EFPIA Patient W.A.I.T. Indicator 2021 Survey, 3. EFPIA, 2020
REFERENCES:
http://www.amchameu.eu/Healthcare-CEE
REPORT: http://www.amchameu.eu/node/14890